Welcome to Northwest Surgical Specialists, Foot and Ankle Care Pain Management Center
Northwest Surgical Specialists is a Multi Medical Practice & Surgical Care Center providing excellent care to adults, senior citizens and children of all ages.
Northwest Surgical Specialists
Northwest Surgical Specialists is a Multi Medical Practice & Surgical Care Center providing excellent care to adults, senior citizens and children of all ages.
Our facility providing excellent care to adults, senior citizens and children of all ages. Our friendly staff and doctors are available to help you with your foot and ankle ailments no matter how severe they may be. In our Hoffman Estates office we also provide Interventional Pain Management with x-ray imaging to deliver precision pain relief.
What we treat

Sports-Related Injuries
Injections are a treatment option for athletes whose joint or tendon injuries have not responded to conservative treatments.
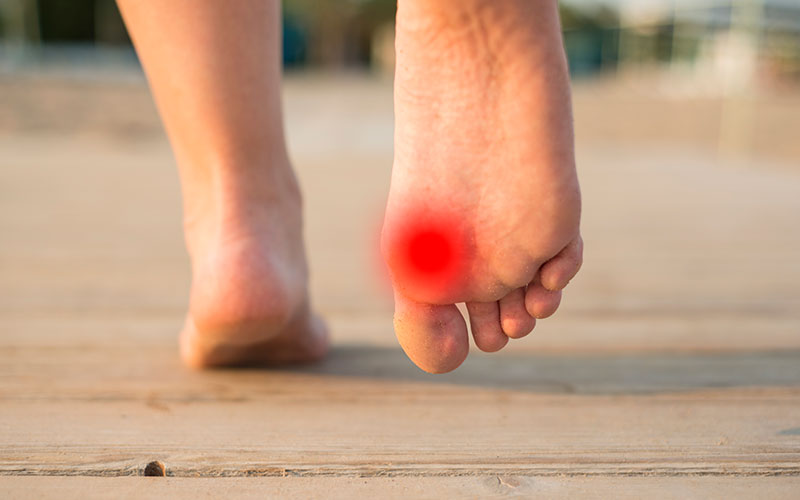
Plantar Warts
Plantar warts are small growths that usually appear on the heels or other weight-bearing areas of your feet.

Bunions
A bunion is a painful bony bump that develops on the inside of the foot at the big toe joint.

Back and Neck Pain
For pain relief, injections can be more effective than an oral medication because they deliver medication directly to the anatomic location that is generating the pain.

Custom Orthotics
Custom orthotics are specially-made devices designed to support and comfort your feet. Prescription orthotics are crafted for you and no one else.

Athlete's Foot
Athlete’s foot – also called tinea pedis – is a contagious fungal infection that affects the skin on the feet and can spread to the toenails and sometimes the hands.
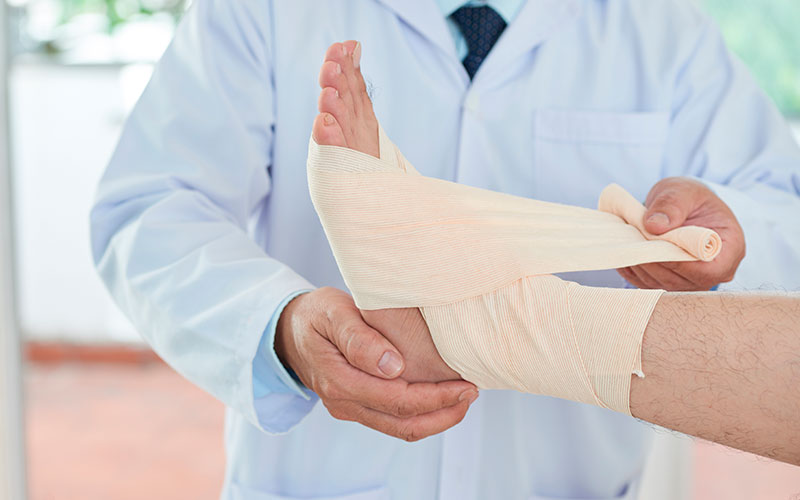
Diabetic Foot Care
People with diabetes and specific foot deformities should buy shoes that match the width of their foot, perhaps with extra depth.
Surgical Center
Laoreet id donec ultrices tincidunt arcu sed cras ornare arcu dui. Donec ultrices tincidunt arcu sed cras ornare arcu dui.
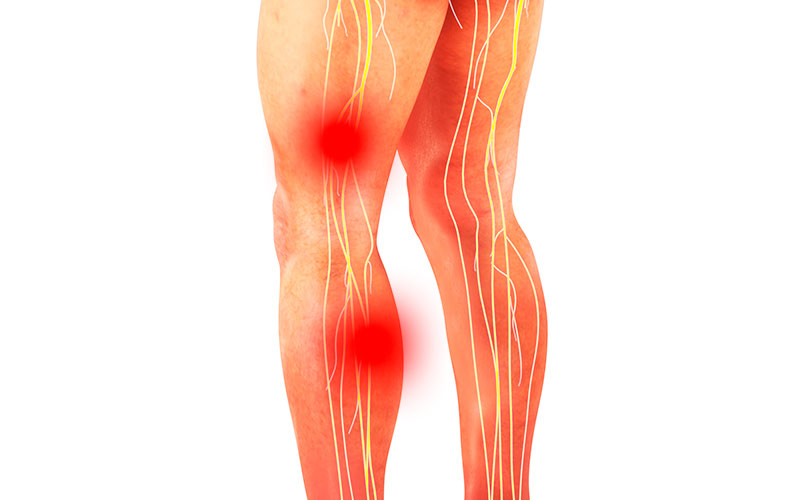
Sciatica
Your sciatic nerve starts at your spinal cord, runs through the hips, and branches down into each leg, and it is the sciatic nerve that allows you to control and feel your legs.

Worker’s Compensation Injuries
According to the Bureau of Labor Statistics, there are over 12 million work-related injuries every year, accounting for 20% of all injuries sustained in the US.
Facet Joint Arthritis
Facet joints are small joints at each segment of the spine that provide stability and help guide motion.
Stories from our patients
We are very proud of the service we provide and stand by every product we carry. Read our testimonials from our happy customers.
Schedule a doctor's appointment
Our friendly schedulers will respond to your request within 48 hours to confirm your appointment.
